|
Heel Pain and the Proper Diagnosis
Milton J. Stern, DPM FACFAS
Almost all of the patients that come to
our office complaining of heel pain think that they have a heel
spur. Some do, some don’t but almost ALL of them are not having pain
from the heel spur itself.
We know that a heel spur is a bony projection from the large bone of
our heel called the calcaneous. Bone does not have any nerve endings
so it can’t cause a lot of pain. Most pain in our heel is from
damage or inflammation of the soft tissue of the heel.
Not all heel pain is treated the same. Getting the right diagnosis
is essential for proper treatment. Once we determine the exact cause
of the heel pain, we can start the proper treatment plan to help
reduce the pain. Not diagnosing the cause properly and starting the
wrong treatment can sometimes make the heel condition more painful.
This is not always that easy. There are many health providers who do
not understand the different causes of heel pain and start the wrong
treatment making the condition worse.
We believe there are four major problems with our
heels that cause ninety percent of all heel pain. Each one has
either a different location or onset of pain. By determining the
exact location of the pain and when in the day the pain is the
worst, we can usually diagnose the problem with a high level of
accuracy.
The four major problems that can affect the heel are plantar
fascitis, heel bursitis, retrocalcaneal bursitis and heel neuritis.
It is very important to note that there are other etiologies of heel
pain. These include but are not limited to rheumatoid arthritis,
gout, psoriasis, fractures of the heel, growth plate abnormalities
in children and bone tumors. It is essential to note that if your
heel pain does not get better and seems to be getting worse; these
other problems must be ruled out.
Every treatment plan has the ultimate goal of reducing the patient’s
pain. We treat heel pain on three different levels in the office. We
use injectable medication for three weeks, oral medication for four
weeks but the secret to help make these medications work is
to control the forces that made the heel hurt in the first
place. If you do not control these forces
then no
other treatment plans including medication, injection, stretching
exercises or physical therapy will be 100% effective. This means
putting something in the shoe that will control each of the four
major problems that can affect the heel.
We will talk about each of the four problems, how we treat
them in the office and what you can do a home.
Plantar
Fascitis
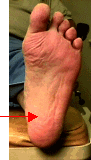 Plantar
fascitis is the most common heel pain syndrome that we see in our
office. It is also the easiest to treat and has the highest success
rate. Ninety percent of all people with this condition get better
with conservative care. The plantar fascia is a thick ligament that
runs from the heel bone to the toes. It is a major supporter of the
arch. Anything that puts increased pressure on the arch can start
this condition. The pain is located on the inside of our foot right
at the edge of where we start to feel our heel bone. The first step
in the morning is the worst. After a few steps it seems to get
better. The pain returns after we sit back down for a short time and
go to stand back up again. Plantar
fascitis is the most common heel pain syndrome that we see in our
office. It is also the easiest to treat and has the highest success
rate. Ninety percent of all people with this condition get better
with conservative care. The plantar fascia is a thick ligament that
runs from the heel bone to the toes. It is a major supporter of the
arch. Anything that puts increased pressure on the arch can start
this condition. The pain is located on the inside of our foot right
at the edge of where we start to feel our heel bone. The first step
in the morning is the worst. After a few steps it seems to get
better. The pain returns after we sit back down for a short time and
go to stand back up again.
Conservative treatment renders ninety percent of
all patients pain free. In our office on a first visit we usually
take x-rays to rule out any other problems. We recommend a combined
treatment of a series of three injections of a cortisone type
medication at weekly intervals to treat the acute inflammation. We
recommend a non-steroidal oral medication to be taken concurrently
for four to five weeks. This treats the chronic inflammation.
The secret to this condition is to control
the arch. We control the arch and the
plantar fascia by taping the foot so as to not let it stretch out.
For long term control we place an orthotic(arch support) in the
shoe. This can be an
over the counter or a more
custom fitted arch support.
At home you can try a couple of simple things. After any prolonged
walking or being on your feet all day you should ice the bottom of
your foot. This helps decrease the amount of inflammation. Take
aspirin, not Tylenol, two pills twice a day for four weeks. You can
also try Motrin or Aleve. If this upsets your stomach stop taking
the medication. Try an over the counter arch support to control some
of the stretching of the plantar fascia. A gym shoe especially a
high top one will control not only the plantar fascia but also heel
motion and the amount of shock the heel gets in normal walking.
Since 90% of all patients get better with
conservative care, it rarely requires surgical intervention. The
surgery consists of releasing the plantar fascia from the calcaneous.
This can be accomplished by a very small incision on the inside of
the heel. A new treatment modality is now available.
Extracorporeal shock wave therapy
uses a machine similar to the one used for kidney and gallstones.
This machine is indicate only for chronic proximal plantar fascitis.
See
Foot News for more information.
Heel
Bursitis
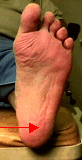 Heel
bursitis is a condition where the normal padding under the heel is
defective. As we walk we traumatize our heel. Many of our modern
shoes have no cushioning under the heel especially a woman’s flats.
The body wants to protect itself so it creates something to help
with the cushioning. This is a fluid filled sack called a bursa. The
symptoms are exactly the same as with plantar fascitis. There is
morning pain when you first get out of bed and pain after you sit
for a while and get back up. The only difference is the location of
where the pain is. Instead of on the inside of the arch area the
pain is directly under the heel. Heel
bursitis is a condition where the normal padding under the heel is
defective. As we walk we traumatize our heel. Many of our modern
shoes have no cushioning under the heel especially a woman’s flats.
The body wants to protect itself so it creates something to help
with the cushioning. This is a fluid filled sack called a bursa. The
symptoms are exactly the same as with plantar fascitis. There is
morning pain when you first get out of bed and pain after you sit
for a while and get back up. The only difference is the location of
where the pain is. Instead of on the inside of the arch area the
pain is directly under the heel.
Conservative care helps about seventy-five percent of our patients
with their pain. On the first visit to our office we take x-rays to
rule out any other problems. We recommend a series of three
injections of a low dose medication into the bursal sack. Again we
use an oral non-steroidal medication for four to five weeks
duration. The secret to this
condition is to control heel strike.
Instead of controlling the arch we want to
protect the heel from further trauma. We recommend a heel cup of a
soft material, usually a viscoelastic compound with a very soft
center. The
UCO heel cup is the best one we have found to
date.
At home you can again apply ice after any exercise or prolonged
walking. Take aspirin, Motrin or Aleve as directed. Protecting your
heel is essential. This is done by wearing shoes with soft insoles
and putting something soft in your shoes. Going barefoot around the
house makes this condition worse.
Surgery on this condition is a little more difficult than the
plantar fascia. Because the bursal sac is directly below the
calcaneous, to get proper exposure you need to make a plantar
incision. Plantar incisions can cause problems of there own
including scarring, protracted pain and incision breakdown. A
medial approach with facial release has been more beneficial.
Bursal sacs can be adventitious and form anywhere so recurrence is
possible.
Retrocalcaneal Bursitis
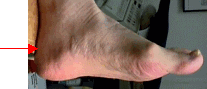 This
is the only condition we will talk about that affects the back of
the heel. Where the Achilles tendon attaches to the heel bone is
the site of this condition. The pain is similar to plantar fascitis
and heel bursitis in that the morning is the time the pain is the
worst. After we sit and stand back up it can hurt again. There is
usually a prominence of bone we can feel in the back of our heel.
This condition affects women to a greater extent because of the type
of shoes they wear. This
is the only condition we will talk about that affects the back of
the heel. Where the Achilles tendon attaches to the heel bone is
the site of this condition. The pain is similar to plantar fascitis
and heel bursitis in that the morning is the time the pain is the
worst. After we sit and stand back up it can hurt again. There is
usually a prominence of bone we can feel in the back of our heel.
This condition affects women to a greater extent because of the type
of shoes they wear.
Conservative care helps only
seventy percent of our patients. On a first visit to the office we
take special x-rays of the heel. We recommend a stretching program
to our patients to try to reduce the inflammation and stretch out
the Achilles tendon. We do not give any injections of steroid to the
back of our heels. This can weaken the Achilles tendon causing it to
detach. Our treatment plan consists of a stretching program and oral
anti-inflammatory medication for four weeks. There is a new form of
physical therapy we have been using that has been very helpful in
reducing the pain. This is called acetic acid iontophoresis. It is
more successful when used early on in the treatment process.
The secret to this condition is to control
heel strike, heel motion in the back of the shoe and physically
protect the back of the heel from the shoe.
This is done by using a
Tuli’s heel cup. The Tuli's heel cup protects
the back of the heel from irritation by the shoe. If this does not
give enough relief then a custom orthotic with a deep heel cup is
recommended.
At home you can try a few things. Using a high top gym shoe protects
the back of our heel and controls heel motion. Again try aspirin,
Motrin or Aleve as directed if you can take tolerate the medication.
Ice your Achilles tendon after exercise. Start a stretching program
to the back of your leg. Start using a Tuli’s heel cup immediately.
The surgeries for this condition are pretty successful. They
require removing the bone spurs from the back of the heel and
possibly remodeling the heel bone. The Achilles tendon attaches to
the bone in the back of the heel. If too much of the Achilles has
to be removed from the bone it has to be reattached with metal
anchors. The recovery period form this procedure can be up to 10
weeks.
Heel Neuritis
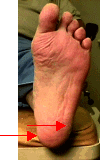 This is the most commonly misdiagnosed condition of the heel. Since
we treat a lot of heels we see more of this condition than any
other. The reason that this number is so high is that with any of
the other conditions most patients respond to the conservative
treatment plans. If heel neuritis is misdiagnosed as plantar
fascitis and a rigid type arch support is used the condition will
get worse. Getting the proper diagnosis is essential. Only forty
percent of patients with this condition get pain free. This is the
worst condition of the heel to have and it is the most painful.
Although there still might be some morning pain and pain when rising
the hallmark of this condition is that the pain never goes away and
progressively gets worse as the day goes on. The pain is very sharp
and at times can cause intense burning. Sometimes there is a sharp
shooting pain that travels up the leg. The pain is far more severe
than any of the other conditions of the heel. Many patients have so
much pain as they walk that they transfer the weight from their heel
to their toes. This can cause increased pain in the ball of the foot
and make the Achilles tendon behind the heel very sore. There are
two different nerve roots that can be involved. The first is on the
inside of the foot. The other, which is more severe, is on the
bottom and outside of the foot.
This is the most commonly misdiagnosed condition of the heel. Since
we treat a lot of heels we see more of this condition than any
other. The reason that this number is so high is that with any of
the other conditions most patients respond to the conservative
treatment plans. If heel neuritis is misdiagnosed as plantar
fascitis and a rigid type arch support is used the condition will
get worse. Getting the proper diagnosis is essential. Only forty
percent of patients with this condition get pain free. This is the
worst condition of the heel to have and it is the most painful.
Although there still might be some morning pain and pain when rising
the hallmark of this condition is that the pain never goes away and
progressively gets worse as the day goes on. The pain is very sharp
and at times can cause intense burning. Sometimes there is a sharp
shooting pain that travels up the leg. The pain is far more severe
than any of the other conditions of the heel. Many patients have so
much pain as they walk that they transfer the weight from their heel
to their toes. This can cause increased pain in the ball of the foot
and make the Achilles tendon behind the heel very sore. There are
two different nerve roots that can be involved. The first is on the
inside of the foot. The other, which is more severe, is on the
bottom and outside of the foot.
Conservative care helps only sixty percent of patients get
pain free. On the first visit we review x-rays, recommend a
treatment of a series of three injections of a steroid type compound
and oral anti-inflammatory
medication for four weeks.
The secret to this condition is
again to control heel strike.
We again recommend a
UCO heel cup. This heel cup works by controlling the shock of
the heel hitting the ground. If this does not give enough relief of
the pain then we recommend our
newly designed orthotic that not only
controls heel strike but the shearing forces of the heel as in
inverts and everts during walking. We have had great success with
this device.
At home you treat this condition the same as heel bursitis. Apply
ice after any exercise or prolonged walking. Take aspirin, Motrin or
Aleve as directed. Protecting your heel with a UCO heel cup is
essential in this condition. Anything that can injure your heel must
be avoided especially going barefoot.
Surgery for these two conditions are a little more technical. The
medial calcaneal nerve is a sensory nerve only. It has no motor
function. If the pain becomes unbearable then you can stop the pain
by stopping the nerve from functioning. This is done by either
chemical neurolysis with alcohol or possible surgical transection.
The first branch of the lateral plantar nerve is another story. It
has a motor function in the foot so chemical neuroysis or
transection is not recommended. Open reduction is required. This
is only 60% successful.
Combinations
This is where it can get a little
confusing. Many patients don’t present with just one of the four
heel syndromes. Many times they will present with two and even three
of the conditions at the same time. Usually plantar fascitis, heel
neuritis and heel bursitis will be in combination. Most of the time
retrocalcaneal bursitis is not in combination with the other heel
syndromes. So sometimes there is morning pain, which eases off a
little after walking, but there is increased pain as the day goes
on. It is important to treat the condition with the worst prognosis
first. We will treat heel neuritis as the primary complaint followed
by heel bursitis and plantar fascitis. Heel neuritis and heel
bursitis can pretty much be treated the same.
The problem comes in when you have plantar facial
pain with either or both heel neuritis and heel bursitis. You treat
the neuritis or bursitis as the primary complaint. Using the UCO
heel cup and taking aspirin will help both the neuritis and the
bursitis pain. When you use the UCO heel cup it raises your heel up
a little and that stretches out the plantar fascia potentially
causing it to get worse. If you use a regular orthotic that is hard
on the top, the plantar facial pain will go away but the heel
neuritis and heel bursitis will become unbearable. If after you try
the UCO heel cup are still having increased plantar facial pain you
might be a candidate for our
newly designed custom orthotic, which controls the plantar
fascia and cushions the heel. This orthotic is the only thing we use
to treat combination heel syndromes involving the plantar fascia .
This orthotic has greatly improved our success rate with combination
heel syndromes.
|